Securing sustainable funding for viral hepatitis elimination plans: Key elements for successful European and national strategies to eliminate Hepatitis C in Europe
Editor-in-Chief, Prof Angelos Hatzakis, MD PhD
Contents
On 6 June 2018, the Hepatitis B and C Public Policy Association (HepBCPPA), held the 2nd European Union (EU) HCV Policy Summit entitled “Securing sustainable funding for hepatitis elimination plans” in Brussels, Belgium. This high-level conference represented the next major step towards the elimination of hepatitis C in Europe. Τhe main stakeholders in the field of hepatitis C in attendance were: clinicians, patient associations, representatives of key institutions and regional bodies from across Europe to present the case for a European elimination strategy for hepatitis C in the presence of EU and national policymakers (1,2).
During the Summit, the case was made for the need to ensure that all elements involved in the cost of HCV elimination: surveillance, monitoring, awareness, screening, prevention and treatment programs, are affordable (1,2). The European institutions and stakeholders represented were the European Parliament Friends of the Liver MEP group, the European Liver Patients’ Association (ELPA), the European Association for the Study of the Liver (EASL), the CORRELATION Network & European Civil Society Forum, the Centre for Disease Analysis Foundation (CDA), and the World Health Organization (WHO). In addition, several members from national parliaments attended the summit. In total, 90 delegates attended the event with 29 different nationalities present.
It is estimated that 3 million people are infected with hepatitis C virus (HCV) in the European Union (EU), but the majority of these individuals remain undiagnosed and untreated. Further, during recent years, migration has compounded the response, since 2.1 million migrants are estimated to be anti-HCV positive. Additionally, hepatitis C is highly prevalent and under addressed in Eastern Europe. In 2013, the introduction of highly effective treatments for HCV with direct acting antiviral (DAAs) therapy created an unprecedented opportunity to cure almost all patients and eliminate the disease, while serving as transmission prevention. However, in many settings, HCV elimination represents a serious challenge for countries’ health spending. On 6 June 2018, the Hepatitis B and C Public Policy Association held the 2nd EU HCV Policy summit. It was emphasized that key stakeholders should work collaboratively since only few countries in the EU are on track to achieve HCV elimination by 2030.
Global burden of HCV: need for action to overcome barriers
Hepatitis C remains a global health problem and it continues to have a large human, social and economic impact (3). According to the most recent WHO global hepatitis report, 71 million people are chronically infected by hepatitis C, and of these, 80% are undiagnosed, mostly because they are asymptomatic and 93% remain untreated (4). Even in countries with high levels of hepatitis C awareness, less than 40% of the infected patients have been diagnosed and an even lower proportion have received antiviral therapy. Unfortunately, the global number of deaths due to hepatitis C continues to rise: more than 1,095 people every day and 400,000 people each year die from HCV-related liver diseases even though HCV is curable with the availability of direct acting antivirals (DAAs)(5). In addition, the population of non-treated HCV-infected people has been ageing – reaching a critical period to develop life-threatening complications (6).
Although HCV continues to spread as a largely “silent pandemic,” its elimination is made possible through the availability of new, safe and effective treatments for HCV with direct acting antivirals (DAAs) and the implementation of prevention practices. However, in the majority of countries, HCV elimination represents a serious challenge for countries’ health budgets as they are faced, for the first time in history, with a fast-acting curative high-cost treatment for a widespread, chronic viral disease that offers little risk of resistance or relapse. In addition to treatment costs, the cost of scaling up testing to find the non-identified infected individuals and implementing effective models of care for diverse populations represents additional challenges. On the other hand, the European economic crisis has impacted public health spending more than on any other public life sector with shrinking budgets. On 28 May 2016, WHO published the Global Health Sector Strategy on viral hepatitis, which called for the elimination of viral hepatitis as a public health threat by 2030 and set the targets at two time points (2020 and 2030).
European burden of HCV
It is estimated that 3 million people are infected with hepatitis C in the EU, and of these, 68% are undiagnosed and less than 6% have been treated. In addition, despite the availability of DAAs, 16,000 patients were diagnosed with hepatocellular carcinoma (HCC) and 22,500 deaths related to chronic hepatitis C were recorded in 2017, i.e. every 25 minutes, an HCV-infected person died of liver complications in the EU in 2017 (7).
Hepatitis C represents a major burden in the EU. The cost of inaction is great: 136,000 additional deaths, 90,000 additional HCC cases, and 71,000 decompensated cirrhosis cases are estimated between 2017-2030. Even EU countries with a high treatment rate will not be able to sustain the treatment without universal screening and political will is the main predictor of whether a country will achieve the 2030 elimination targets.
During recent years, migration has become a challenge given that 2.1 million migrants are estimated to be anti-HCV positive (8). Another challenge is hepatitis C in eastern Europe. Currently there is an epidemic exploding in the region and it is driven by injecting drug use, the lack of awareness at all levels (especially political), the absence of surveillance systems, national strategies and limited or no funding for hepatitis programs, and often obsolete management programs (8).
What is the state of play of HCV elimination in the EU?
Currently, few countries in Europe (France, Georgia, Iceland, Italy, Netherlands, Spain, Switzerland and UK) are on track for HCV elimination by 2030.
Fortunately, the actual number of treated patients with hepatitis C has increased over the last few years since DAAs have become available. At this rate, the EU only needs to diagnose 160,000 (from today’s 90,000) and treat 180,000 (from 160,000 today) annually to reach the 2030 WHO elimination target.
In order to achieve the 2030 elimination targets seven requirements are needed: 1) financing of the national elimination program, 2) implementation of harm reduction programs, 3) expand capacity beyond specialists, 4) remove treatment restrictions, 5) implement monitoring & evaluation, 6) implement awareness and national screening programs, 7) implement national linkage to care program.
Eliminating hepatitis C: the impact of the micro-elimination approach (13)
The WHO targets for HCV elimination are challenging, costly and complex. However, the continuum of viral hepatitis services and the retention cascade need simplification similar to those of HIV infection. In addition, it should be recognized that elimination of hepatitis C is still a daunting task for health systems. However, an idea is to break down this cost by subgroup or population, by year, or region, for example. In fact, formidable obstacles to reaching HCV elimination can best be overcome through a micro-elimination approach, which entails pursuing elimination goals in specific populations. Micro-elimination is less daunting, less complex, and less costly than full-scale, country-level initiatives to eliminate HCV, and it can build momentum by producing small victories that inspire more ambitious efforts. The micro-elimination approach encourages stakeholders who are most knowledgeable about specific populations to engage with each other and also promotes the uptake of new models of care (13).
A successful micro-elimination approach should meet the following four criteria, although these criteria may need to be adapted to different epidemiologic situations and geographic settings: a) there should be a plan in order to tailor health resources and services with the aim of overcoming known barriers and achieving high levels of HCV diagnosis and treatment rates in one or more clearly defined populations of interest within a specified timeframe, which can be faster than in the general population, b) the plan sets forth achievable annual targets, basing these on mathematical modeling when relevant to determine the levels of diagnosis and treatment required to progress to the plan’s ultimate elimination targets, c) the plan is developed and implemented through a multi-stakeholder process, with essential participants including government officials, health service providers and civil society representatives and d) progress and outcomes need to be monitored and publicly reported using indicators selected at the outset of the process (14).
Progress report towards elimination by 2030 globally and in Europe (15)
WHO developed the Global Health Sector Strategies, 2016–2021 including three organizing frameworks: universal health coverage (UHC), continuum of health services, and the public health approach (15). To reinforce the commitment of the global goal, members of the EU have endorsed the first European action plan (15). Based on this plan, several regional essential targets should be reached by 2020 regarding prevention, and particularly, testing and treatment. It is encouraging that the number of European countries with national plans increased from 13 in 2013 to 22 in 2017(15). However, several challenges remain, since there is a lack of global donors and commitment in many countries, data is patchy and monitoring systems are nascent, most people living with hepatitis are still undiagnosed, treatment access is limited by regulatory barriers and high prices, particularly for newer antiviral drugs.
Cost of HCV elimination: Direct medical cost, patients reported outcomes and productivity loss
Several studies have shown that patient-reported outcomes (PROs) and work productivity (WP), both important components of comprehensive outcomes assessment, are impaired in HCV infected patients (16). PROs are important surrogate markers of patient experience, and their impairment, especially in the domains of physical functioning and mental health, is the result of the virus replicating itself. Regarding WP, HCV appears to affect absenteeism from work leading to a substantial economic burden to employers (17). As a result, although in 2011 the total direct cost of HCV-related liver disease had been estimated at USD 6.5 billion in the USA (projected to peak at 9.1 billion in 2014), the indirect economic burden of WP loss in the USA has been estimated to be approximately USD 7.1 billion per year and EUR 2.6 billion per year in 5 major European countries (France, Germany, Italy, Spain and United Kingdom) (16,18). Interestingly, PROs and WP are improved during treatment with antiviral therapy with DAAs, and this improvement is sustainable and durable after successful antiviral therapy with DAAs leading to clinical, PRO and economic gains (19).
Cost of screening
Many patients have an advanced clinical stage of liver disease with or without severe complications at the time of diagnosis. For example, in France, 12% of patients had cirrhosis and/or hepatocellular carcinoma at the time of referral at hepatology centres in 2007 (20).
HCV screening guidelines still target only people at high risk of infection, but this approach requires reconsideration in the light of treatment with DAAs, which can be used as a means of prevention, particularly in high-risk populations, such as MSM and PWIDs. For example, DAA treatment can reverse the HCV epidemic over the next ten years among MSM in the UK, particularly for those with recent HCV diagnosis (21). Similarly, in France, treatment with DAAs may have a great impact in reducing the prevalence of HCV infection and liver-related morbidity in PWIDs (22).
In France, considering that the general population aged between 18 and 80, without any known diagnosis of HCV-RNA positivity is about 45 million and assuming that the testing coverage could be 9 million/year, the budget of the implementation of this model over 5 years is estimated to be 869.4 million euros (while the total budget for HCV treatment in 2017 was 735 million euros) (23). Based on these findings, a National Health Strategy was announced in France in 2018 recommending actions in order to strengthen: a) access to hepatitis C treatment for all; b) proximity to screening by rapid diagnostic orientation testing in a combined approach to HIV, HBV and HCV) prevention through innovative “go-to-go” actions to reach priority and bring audiences into the health system.
Is hepatitis C elimination cost-saving?
Globally, treatment with DAAs can reduce the burden of HCV-associated disease by 50%-70% between 2015 and 2050; liver-related deaths (from 767,000 without treatment to 317,000); hepatocellular carcinoma (from 407,000 without treatment to 154,000); and liver transplants (from 63,000 without treatment to 31,000). (24, 25)
Τhe costs for cure decrease steadily over time because more effective therapies are available (26). Interestingly, the lifetime cost of hepatitis C treatment using DAAs is <$30,000 (particularly with the implementation of generic drugs), significantly lower than HIV treatment ($315,000) and primary biliary cholangitis using obeticholic acid ($900,000). More importantly, the cost to gain 1 additional quality-adjusted life year for HIV treatment is < $30,000 (thus, it is cost-effective), for primary biliary cholangitis (using obeticholic acid) is $190,000 (thus, it is not cost-effective), while for hepatitis C treatment (using oral DAAs) is negative (thus, it is cost-saving, i.e. the more we treat the more we save, not only lives but also economically)(24).
Data from the UK have shown that in an elimination scenario, compared to the current status quo, an initial investment is needed, but then a significant reduction in the cost is expected over the next years.
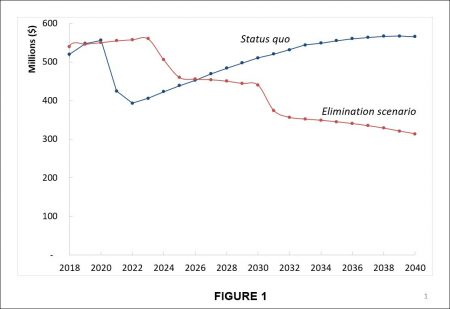
Figure 1. Cost of HCV Elimination versus Status Quo in the United Kingdom over the next twenty years. In the elimination scenario an initial investment is needed, but then a significant reduction in the cost is expected.
Elimination of HCV requires strong collaboration between stakeholders. The plan for HCV elimination should be achievable, sustainable and follow the WHO time frame (27). There is general consensus that one of the crucial factors to achieving this goal is adequate funding for the continuum of care to support the HCV elimination initiative. Financing remains a major barrier and making the treatment affordable is still a major challenge for many European countries.
Innovative financing for HCV elimination (28)
New sources of funding will be required for countries to launch, accelerate and sustain public health responses to eliminate viral hepatitis. These resources will need to be substantial to meet elimination targets. It is true that for HCV elimination, investment is needed over a long period of time (e.g., providing antiviral treatment until 2030), but since HCV is a slow progressive disease, the return on investment will accrue after a long time. Through bond finance, not only can governments release money for public spending, but the maturity period can be adjusted to the timeframe in which the investment produces the desired social/economic benefit. One option could be commercial bonds, which are widely used in the public sector for funding infrastructure projects, while vaccine bonds were developed by the International Finance Facility for Immunization (IFFIm) (29). Another option could be social impact bonds, i.e. a contract with the public sector in which a commitment is made to pay for improved social outcomes that result in public sector savings (e.g., social bond for rehabilitation of incarcerated people and to reduce recidivism) (28).
As George Papandreou, President of the Socialist International, and former Prime Minister of Greece and keynote speaker at the 2nd EU HCV Policy summit mentioned, some European countries have already important experience in creating social bonds and similar financing tools. Other countries may prefer to explore opportunities through cooperation with the European Financial Institutions such as the European Investment Bank. Thus, the EU Commission could prepare the legislative actions, to convincingly motivate the European Investment Bank and other European financial institutions to take this ambitious yet totally realistic project on board (30).
Financing of viral hepatitis elimination in low and middle-Income Countries (31)
Although hepatitis elimination has a positive return on investment– the main problem is the need for upfront investment. An alternative approach could be based on patients who are willing to pay for healthcare expenses (for example in many of the lower middle-income countries, a high proportion of patients of all treatments are currently in the private market) providing that the costs are kept below the catastrophic healthcare expenditure level, while some portion of the population will not be able to pay for their healthcare. This model can be supported by suppliers who are willing to provide price concessions if large volumes are guaranteed, as well as banks and donors who are willing to provide catalytic financing if they have assurances that can get their investment back at the end of the program (31).
The new model would foresee the use of loans instead of donations to support the hepatitis elimination programs. Thus, although the old model based on donations (donations from the few pay for the needs of the many, including for those who could afford some payment), in the proposed new model, patients fund their treatment (small loan from investor, plus funds from many patients, pay for diagnostics and treatment for all, plus repayment to investors).
More efforts are needed to raise awareness of viral hepatitis amongst the general population and general practitioners, and to improve diagnosis of HCV in primary care settings providing sustainable, affordable, universal access to the tools for elimination. It is important to build on support of the European Parliament and to influence the agenda of the next European Commission and the governments of EU Council Presidencies during the transition in 2019-2020 aimed to improve diagnosis and access to treatment amongst defined key groups, such as PWID (12).
However, the economic crisis has led to cuts in funding for harm reduction in many countries. Thus, there is a need to move towards a single-visit hepatitis C diagnosis, instead of the five-visits of the interferon era, in order to decrease the time of diagnosis (from 4-6 weeks or more to no delay) and the rates of lost follow up. The new treatment options give this opportunity, since hospital attendance requirements are evidenced barriers particularly for marginalized populations. In this direction, more efforts are needed to increase screening in risk groups and build capacity for treatment. Political leadership may play an important role in delivering the message of hepatitis C elimination at the political level by keeping hepatitis C high on the political and media agendas (32).
The Call to Action of the 2nd EU HCV Policy Summit recommends that countries have a comprehensive, costed hepatitis C elimination strategy in place to determine their country-level disease and economic burden of HCV by measuring direct and indirect socio-economic costs to improve the response towards HCV elimination and to develop country and population-specific models, to estimate lifetime costs, quality-adjusted life expectancy, and incremental cost-effectiveness ratios of different screening and treatment strategies in comparison with no action. These are necessary to hepatitis elimination programs as hepatitis investment cases.
Innovative financing tools include social impact bonds, with the aim to raise upfront funds for launching new social services and financing prevention services, including harm reduction, contributing to HCV elimination in a sustainable way.
The European Union should recognize the need to engage in HCV elimination by establishing a clear political roadmap and call for European financial institutions to raise public and/or private funding and use elimination programs as development and health systems strengthening tools. Encourage and engage all the stakeholders to collaborate in the development of innovative financing tool.
- Manns MP. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Hatzakis A. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Cooke GS, Andrieux-Meyer I, Applegate TL, Atun R, Burry JR, Cheinquer H, et al. Lancet Gastroenterology & Hepatology Commissioners. Accelerating the elimination of viral hepatitis: A Lancet Gastroenterology & Hepatology Commission. Lancet Gastroenterol Hepatol. 2019 Feb;4(2):135-184
- WHO Global hepatitis report, 2017. Available at: http://apps.who.int/iris/bitstream/10665/255017/1/WHO-HIV-2017.06-eng.pdf.
- Maticic M. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Polaris Observatory. Accesses at: http://www.polarisobservatory.com/.
- Razavi H. HCV Elimination in Europe: Burden Pathways and Cost. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Negro F. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Pimpin L, Cortez-Pinto H, Negro F, Corbould E, Lazarus JV, Webber L, Sheron N; EASL HEPAHEALTH Steering Committee. Burden of liver disease in Europe: Epidemiology and analysis of risk factors to identify prevention policies. J Hepatol. 2018 Sep;69(3):718-735
- Buşoi CS. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Lazarus JV, Stumo SR, Harris M, Hendrickx G, Hetherington KL, Maticic M, Jauffret-Roustide M, Tallada J, Simojoki K, Reic T, Safreed-Harmon K; Hep-CORE Study Group. Hep-CORE: a cross-sectional study of the viral hepatitis policy environment reported by patient groups in 25 European countries in 2016 and 2017. J Int AIDS Soc. 2018 Apr;21 Suppl 2:e25052.
- Reic T. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Lazarus JV. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Lazarus JV et al. The micro-elimination approach to eliminating hepatitis C: strategic and operational considerations. Seminars in Liver Disease, 2018; Aug;38(3):181-192.
- Mozalevskis A. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Younossi ZM. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Younossi ZM, Birerdinc A, Henry L. Hepatitis C infection: A multi-faceted systemic disease with clinical, patient reported and economic consequences. J Hepatol. 2016 Oct;65(1 Suppl):S109-S119
- Razavi H, Elkhoury AC, Elbasha E, Estes C, Pasini K, Poynard T, Kumar R Chronic hepatitis C virus (HCV) disease burden and cost in the United States. Hepatology. 2013 Jun;57(6):2164-70.
- Younossi ZM, Papatheodoridis G, Cacoub P, Negro F, Wedemeyer H, Henry L, Hatzakis A. The comprehensive outcomes of hepatitis C virus infection: A multi-faceted chronic disease. J Viral Hepat. 2018 Nov;25 Suppl 3:6-14
- Brouard C, Le Strat Y, Larsen C, Jauffret-Roustide M, Lot F, Pillonel J. The undiagnosed chronically infected HCV population in France. Implications for expanded testing recommendations in 2014. PLoS One. 2015 May 1;10(5):e0126920.
- Martin NK, Thornton A, Hickman M, Sabin C, Nelson M, Cooke GS, Martin TCS, et al. Can Hepatitis C Virus (HCV) Direct-Acting Antiviral Treatment as Prevention Reverse the HCV Epidemic Among Men Who Have Sex With Men in the United Kingdom? Epidemiological and Modeling Insights. Clin Infect Dis. 2016 May 1;62(9):1072-1080.
- Cousien A, Tran VC, Deuffic-Burban S, Jauffret-Roustide M, Dhersin JS, Yazdanpanah Y. Hepatitis C treatment as prevention of viral transmission and liver-related morbidity in persons who inject drugs. Hepatology. 2016 Apr;63(4):1090-101.
- Deuffic-Burban S. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Chhatwal J. Is hepatitis elimination cost saving? Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Chhatwal J, Wang X, Ayer T, Kabiri M, Chung RT, Hur C, et al. Hepatitis C Disease Burden in the United States in the era of oral direct-acting antivirals. Hepatology. 2016 Nov;64(5):1442-145.
- Chhatwal J, Chen Q, Kanwal F. Why We Should Be Willing to Pay for Hepatitis C Treatment. Clin Gastroenterol Hepatol. 2015 Oct;13(10):1711-3.
- Peck-Radosavljevic M. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Chhatwal J. Innovative financing of HCV Elimination. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Crocker-Buque T, Mounier-Jack S. The International Finance Facility for Immunisation: stakeholders’ perspectives. Bull World Health Organ. 2016 Sep 1;94(9):687-693.
- Papandreou GA. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Razavi H. Financing solutions for hepatitis elimination in low- and middle-income countries. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
- Schatz E. Presentation at 2nd European Union (EU) HCV Policy Summit 2018.
Call to Action to “Secure sustainable funding for viral hepatitis C elimination plans”
The hepatitis C virus (HCV) is a global public health threat with significant morbidity and mortality. Due to its asymptomatic nature, it is also a silent epidemic with an estimated 71 million infected globally, but only 20% diagnosed(1,2).
In 2013, the introduction of new, safe and effective treatments for HCV created an opportunity to eliminate the disease. However, in some settings, this development represents a serious challenge for countries’ health spending as they are faced, for the first time in history, with a fast-acting curative treatment for a widespread chronic viral disease which offers little risk of resistance or relapse. In addition to treatment costs, the cost of scaling up testing to find the non-identified infected individuals and implementing effective models of care for diverse populations, represent an additional challenge.
Greater efforts are needed to ensure that all elements of cost of HCV elimination, which include surveillance, monitoring, awareness, screening, prevention and treatment programs, are affordable. Preliminary data suggest that the WHO HCV elimination strategy may be cost saving for many countries(3, 4). That is the savings related to preventing and treating HCV may exceed the cost of HCV elimination, providing good value for money given the high initial spending. Strategic Direction 4 of the WHO Global Health Sector Strategy on Viral Hepatitis 2016-2021 “Financing for sustainability”(5) sets out financing recommendations for a sustainable hepatitis response, outlining actions to raise revenue to pay for viral hepatitis interventions and services, set-up financial risk protection, and improve efficiency in the use of health system resources.
On 17 February 2016, the launch of the HCV Elimination Manifesto “Our vision for a Hepatitis C-free Europe”, provided a starting point for action to make HCV and its elimination in Europe an explicit public health priority(6, 7). With patients, civil society groups and other relevant stakeholders directly involved in developing and implementing HCV elimination strategies, now is the time to take the next step further and make the HCV elimination affordable.
We, the signatories of the Call to Action “Secure sustainable funding for hepatitis C elimination plans” are committed to HCV elimination in Europe.
In line with the 2015 United Nations’ General Assembly Resolution “Transforming our world: the 2030 Agenda for Sustainable Development”, in line with the Sustainable Goal 3 Good Health and Well-Being and its Target 3.3 to Fight Communicable Diseases, in line with the 2014 World Health Assembly’s Resolution 67.6 on hepatitis, in line with the 2016 HCV Elimination Manifesto, in line with the WHO Global Health Sector Strategy on Viral Hepatitis 2016-2021 “Towards ending viral hepatitis”, and in order to encourage policy-makers to fulfil the Strategic Direction 4 of the WHO Global Health Sector Strategy on Viral Hepatitis 2016-2021, and make HCV elimination affordable, we are calling on the European decision makers to:
- Ensure that countries have a comprehensive, costed hepatitis C elimination strategy in place, including a comprehensive monitoring along with the cascade of care in line with the criteria developed by ECDC and WHO Europe;
- Determine their country-level disease and economic burden of HCV by measuring direct and indirect socio-economic cost to improve the response towards HCV elimination, paying attention to the close link between HCV and HIV in some populations;
- Develop country and population-specific models, as viral hepatitis investment cases, to estimate lifetime costs, quality-adjusted life expectancy, and incremental cost-effectiveness ratios of different screening and treatment strategies with comparison with no action;
- Allocate sufficient resources for training and research, developing robust models of care for tackling HCV, and urgently and effectively fulfil Strategic Directions 2, 4 and 5 of the WHO Global Health Sector Strategy;
- Recognize the need for the European Union to engage in HCV elimination by establishing a clear political road map and call for European financial institutions to raise public or private funding and use elimination programss as a development tool;
- Encourage and engage all the stakeholders to collaborate in the development of innovative financing tools like social impact bond and others, with the aim of launching new social services and financing prevention services, including harm reduction, contributing to HCV elimination in a sustainable way;
- Exchange and implement best practices on funding healthcare and HCV elimination, including via micro-elimination approaches(8) , at the national, regional and local levels to meet the WHO elimination goals by 2030 and preferably much earlier.
Endorsed by:

References
- WHO Global Hepatitis Report 2017.
- The Polaris Observatory HCV Collaborators. Global prevalence and genotype distribution of hepatitis C virus infections in 2015: a modelling study. Lancet Gastroenterology Hepatology 2017 Mar,2(3):161-176.
- Kondili L et al. Modeling cost-effectiveness and health gains of a “Universal” versus “Prioritized” hepatitis C virus treatment policy in a real-life cohort. Hepatology 2017 Dec;66(6):1814-1825.
- Chhatwal J. “Is hepatitis C elimination cost saving?” 2nd EU HCV Policy Summit, Brussels 2018.
- Global Health Sector Strategy on viral hepatitis 2016-2020. WHO, 2016.
- Action plan for the health sector response to viral hepatitis in the WHO European region. WHO, 2017.
- Papatheodoridis G. V. et al. Summit review: HCV Policy Summit Hepatitis C: The Beginning of the End Key elements for successful European and national strategies to eliminate HCV in Europe, Journal of Viral Hepatitis, Volume 25, Issue S1, 2018
- Lazarus JV, Wiktor SZ, Colombo M, Thursz M on behalf of the EASL International Liver Foundation. Micro-elimination – a path to global elimination of hepatitis C. Journal of Hepatology, July 2017.
Prof. Angelos Hatzakis is pleased to announce that the full article arising from the 2nd EU HCV Summit has been accepted for publication in Liver International.



